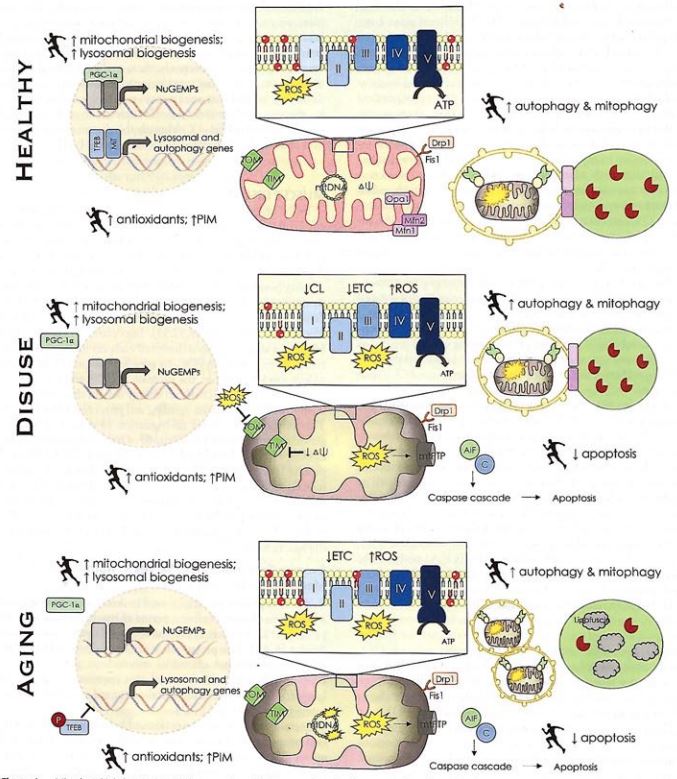
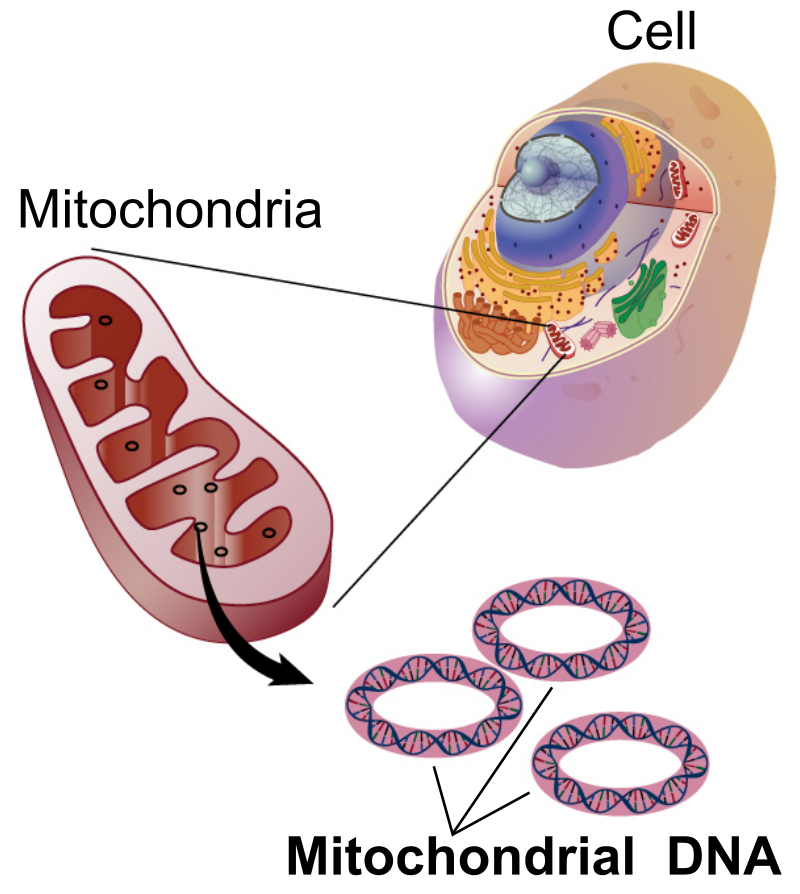
The mitochondria is the 'powerhouse' of the cell. It's DNA is derived from the female side of the genetic inheritance. They exist in two areas of muscle - beneath the sarcolemmal membrane and in the intermyofibrillar region. Together they form the mitochondrial reticulum. Two processes exist, fusion and fission. Fusion of the inner membrane (IM) results in expanding and elongating the mitochondrial reticulum, with more complex and extensive morphologies associated with healthy, exercise trained individuals. Functionally, this allows greater metabolic flexibility, lipid metabolism and greater distribution of mtDNA and metabolites throughout the reticulum. In contrast, fission involves removing portions of the reticulum which have become dysfunctional, limiting the affects of toxic by-products such as ROS (reactive oxygen species), or mtDNA mutations. Structurally, the IM has varying degrees of internal folding, known as cristae, whose surface area determines the effectiveness of the electron transport chain (ETC). Cristae density is often an indication of mitochondrial quality, characterised by exercised individuals.
Ageing
After the age of 30 results in a 10% reduction in aerobic capacity each decade. Whereas, after the age of 40, a 1% reduction of strength occurs annually, which accelerates in the 6th decade of life with inactivity. The latter is known as sarcopenia.

The ageing process (AKA 30 years of age onwards), in the presence of high ROS (reactive oxygen species) and/or damaged mitochondrial DNA, can induce widespread mitochondrial dysfunction. In the healthy cell, mitophagy results in the removal of dysfunctional mitochondria and related material. In the absence of functional removal of unwanted mitochondrial material, a retrograde and anterograde signalling process is potentially instigated, which results in both motor neuronal and muscle fibre apoptosis (death) (Alway, Mohamed, Myers 2017, Ex Sp Sc Rev, 45, 2, 58-69). This process is irreversible. Investigations in healthy populations, have shown that regular exercise improves the ability to cope with regular oxidative stress by the buffering and 'mopping up' of ROS agents which are induced as a result of exercise. It is plausible and highly probable that regular exercise, throughout life, can mitigate against muscle fibre death (Sarcopenia). Importantly, this process of muscle fibre death can commence in the 4th decade of life, and be as much as 1% per year. Reduction of muscle mass can result in immune and metabolic compromise, including subclinical inflammation, type II diabetes as well as the obvious reduction in functional capacity for activities of daily living.
Exercise is muscle mitochondrial medicine during ageing
An elevation in the proportion of dysfunctional mitochondria within muscle with age could be a consequence of reduced biogenesis or impaired removal via mitophargy. The stability of the precursor proteins in the cytosol is reduced in aged muscle, thus providing less substrate for biogenesis. Lysomal dysfunction and the inability to remove damaged organelles and other deficits are reversed through exercise.
A review by Oliviera An et al (2021 Ex Sp Sc Rev, 49, 2, 67-76) considered exercise at a potent therapeutic modality through the stimulation of mitochondrial biogenesis through a key regulator PCG-1aplha, as well as a potent stimulator of mitophagy, whereby damaged mitochondria are removed from the reticulum. Ageing, in the presence of disuse, is known to induce poor muscle oxidative status and metabolic inflexibility. For example, chronic contractile activity (CCA) reverses accelerated ROS production, evident in aged muscle, and increases transcription of PGC-1alpha toward levels found in younger individuals. Additionally, exercise has been shown to increase lysosomal content irrespective of age. Mitophagy flux elevated with age is reduced with exercise.
Mitochondria are highly dynamic, interconnected organelles that continuously undergo events of renewal, removal and reorganization. The balance between biogenesis and mitophagy determines 'turn over' and hence the quality and quantity of mitochondria. In the absence of exercise, fission-fusion regulatory imbalances occur.
Exercise pre-conditioning
Exercise preconditioning is used to describe exercise induced changes before a period of inactivity, which serves to protect the skeletal muscle against atrophy and dysfunction through disuse. This protection is achieved through
- increased cytosolic and mitochondrial antioxidants and chaperones
- increasing mitochondrial gene expression and protein levels
- reduced signalling toward apoptotic and atrophy pathways
Optimal approach to load progression during strength training in older adults
Three dominant approaches exist to progression and exercise training
- perceived exertion (RPE)
- target repetitions (incl. repetitions to failure (RM), repetitions in reserve (RiR)
- % of maximum (%1RM)
It has been established that repetitions to failure for sports specific training is highly effective in some populations, however in older adults it may induce DOMS or worse still function-limiting-injuries. Older peoples perception of exercise are among the major determinants whether a person will continue their exercise program. Too slow progression or too little load can be as unmotivating as an injury from repetitions to failure. Lower intensities may lead to higher adherence rates and feelings of pleasure. But what is too little and too much? Buskard et al (2019, Med Sc Sp Ex, 51, 11, 2224-2233) determined that all forms of progressive exercise improved muscular strength and functional capacity. Moreover the RPE method was significantly more tolerable and enjoyable than the RM, RiR, and %1RM methods. However, this may only hold true for the first 6 months of a training regime, after which time, the individual has become accustomed to the routine of exercise and hence may perceive greater loads as more beneficial with reduced side effects. The latter is speculative but anecdotally appears to be true in some sub-populations involved in competitive exercise.
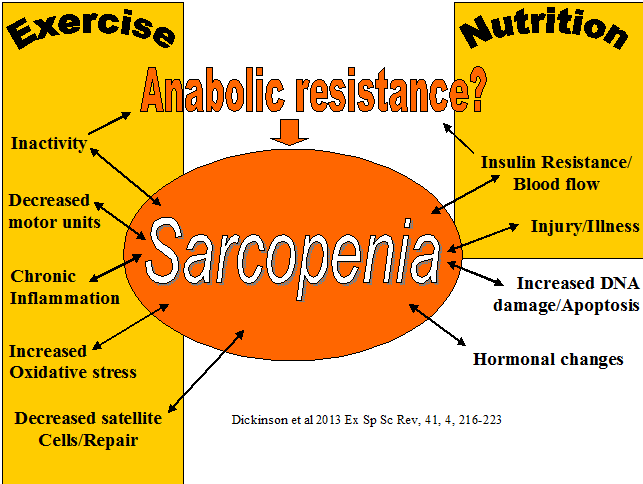
See : Sarcopenia and Aging
Use of chaos theory to load progression and immune integrity during COVID-19
Since the onset of COVID-19 many of us have asked why are there so few antivirals? The answer boils down to biology, and specifically the fact viruses use our own cells to multiply. This makes it hard to kill viruses without killing our own cells in the process. So how do we ensure cell survival, whilst priming the immune system to make antigens for its defence system. What does this even mean? Can exercise be an answer to reduce the extent of our immune response if exposed to COVID-19? Will knowing why exercise is good for our immune system motivate people to exercise more?
During this time of crisis, we've been told to exercise. Exercise for physical and mental well-being. Whether in partial 'lock down' or 'full lock down' or 'opening up', exercise is still important. But Why? How do chaos theory and non-linear dynamics explain movement and the immune system?
We were born from the chaotic fire of genesis. Laws of thermodynamics dictate our existence. Evolution of heat shock proteins (HSP) means that we are our immune system. Today, human multi-cellular life is still totally dependent on our unicellular ancestors and their components. Trillions of species and bacteria in the gut (flora) and skin alone, associated with immune substances, attest to the importance of unicellular life in the immune system. The abundance of energy species in the gut suggests a nexus with one of the organs most in need of energy, the skeletal muscle. Importantly, muscle cells have more mitochondria than most other cells, so they can readily produce work for movement. Consequently, muscles are an energy system and an immune endocrine organ. Notably, the development from unicellular to multi-cellular life needed movement. A commonality of cellular movement and macro-muscular movements exist.
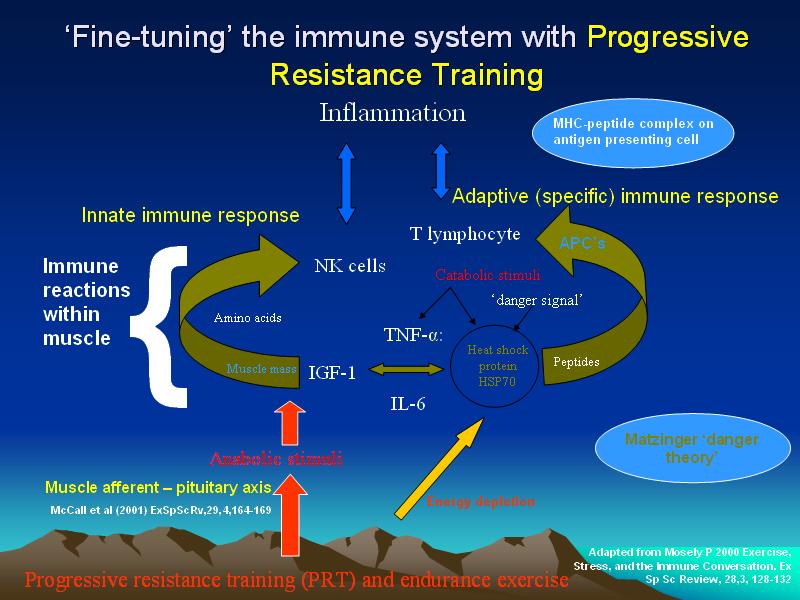
Physiotherapeutic and training interventions must consider the health of the immune system and its ability to deploy and be re-deployed. Training should avoid becoming 'stale' by having enough variety (chaos) to create perturbations in the immune system which induce up and down regulation of immune components. Physiotherapy should be innovative and creative, whereby the physiotherapist additionally considers immune-cognitive aspects of pain and inflammation, when people seek physiotherapeutic intervention after/during a change in their training regime and/or commencement of unaccustomed exercise, or in the presence of immune compromise.
Elsewhere, a synopsis of my past research in the field of biomechanics, pathomechanics, neurophysiology, cognition, immunology, sarcopenia and my current interest in chaos, can be found reading Aging, COVID-19, Chaos, Exercise and the Immune System
p53 and anti-carcinogenic protein deficits
p53 is considered a tumour suppressor protein and drives cellular apoptosis and DNA damage/repair. p53 may also have important functions for basal mitochondrial content and function, whilst the effects of it's reduction or absence, on the mitochondria, has been shown to be reversed with exercise(Oliveira AN 2021, Ex Sp Sc Rev, 49, 2, 67-76)
Published 11 July 2017
Updated : 7 February 2022